Up to ⅓ of patients suffering from epilepsy have a drug-resistant form of this condition. Among the alternative treatment options, one of the most effective and safest is vagus nerve stimulation, also known as VNS therapy. Read more about it in our article.
Listen to the article:
What is vagus nerve stimulation?
Vagus nerve stimulation involves placing a subcutaneous implant attached to the vagus nerve. This device can create electrical impulses that are sent to the brain to correct its abnormal activity. This reduces the number and intensity of epileptic seizures. 1 out of 10 patients managed to get rid of them completely thanks to VNS therapy.
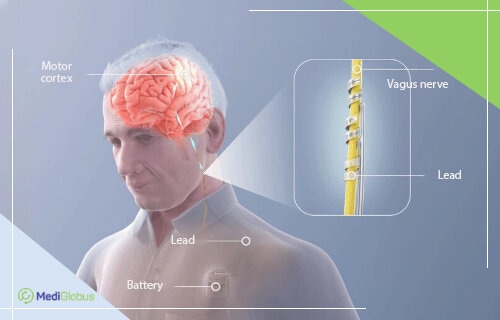
VNS therapy is approved by the FDA and EMA for the treatment of epilepsy. The surgery can be performed on patients of any age.
The method has been in use worldwide since the late 1990s. Today, more than 125,000 people, a third of whom are children, are living with a vagus stimulator. Their experience shows that the method is highly effective and safe. The percentage of postoperative complications after a VNS pacemaker installation is very low, at around 1%. By comparison, another alternative treatment for drug-resistant epilepsy, brain surgery, leads to complications in 5% of cases.
The effectiveness of a vagus stimulator only increases over time. About half of all patients report a positive trend within the first year, while 76% of patients report a decrease in the number of attacks after 10 years.
Stimulation of the vagus nerve helps with epilepsy because it affects the electrical activity of the brain. The regular pulses sent by the machine change the level of neurotransmitters (substances that regulate neural activity), alter EEG and increase blood flow to the brain.
Stimulation of the vagus nerve is an adjunctive therapy. This means that in most cases the patient will continue to take medication, although probably in much lower doses.
The main benefit of VNS therapy is allowing patients to regain control over their own lives.
There are three models of vagus stimulators available today: the standard, AspireSR and SenTiva.
The standard model of vagus nerve stimulator sends electronic impulses up the vagus nerve in doctor-set parameters – usually for 30 seconds every 5 minutes. The device also comes with a special magnet. If you experience an aura – a premonition of an attack – you can put the magnet onto the pacemaker to make it give a pulse right away. In some cases, this may stop a seizure and in others, it may shorten its duration or make it easier to recover from a seizure. Most patients wear such a magnet on their wrist like a bracelet.

AspireSR is a more advanced model, able to sense the onset of a seizure and increase electronic stimulation of the vagus nerve at the same time. The machine reacts to the increased activity of the heart since 82% of patients experience a fast heartbeat before the onset of a seizure. The AspireSR responds to this by sending an electrical impulse to the brain.
SenTiva is the latest generation of vagus nerve stimulators, allowing doctors advanced individual programming of each device. For example, it can be set to deliver stronger impulses at nighttime. Alternatively, the night mode can be set to be weaker so that it will not cause sleep apnea in patients who are prone to the condition. The SenTiva can also be adjusted so that it temporarily does not respond to an increased heart rate during sports activities.
Modern vagus nerve stimulation machines collect information about a patient’s epileptic activity. The treating physician can then use this to select a more personalized and effective epilepsy treatment plan.
New in epilepsy treatment
Doctors are developing vagus nerve stimulators that will not require surgical implantation. In the future, such devices may take the form of an earpiece or a small device that needs to be pressed to the neck.
SIGN UP FOR A CONSULTATION WITH A DOCTOR
Before VNS therapy is prescribed, patients must undergo a thorough neurological diagnosis. Based on its results the doctor will be able to give an opinion and recommendations for treatment. If you are planning to treat epilepsy abroad, all examinations can be carried out at home and the finished results sent to the clinic. Please contact the MediGlobus coordinating physicians for help in organising this.
How does the surgery for a vagus stimulator take place?
At the first consultation with your doctor, you will discuss all the possible benefits, risks and side effects of vagus nerve stimulation. The frequency of subsequent consultations and changes in medication will also be discussed.
A vagus stimulator will be implanted under the skin in the upper chest during surgery under general anaesthesia. The device is similar to a pacemaker. The electrodes will be attached to the vagus nerve. The procedure lasts 60-90 minutes. Patients are usually sent home the same or the next day. A small bump will remain where the stimulator is placed, and just above that on the neck is a scar, which in most patients heals and looks unnoticeable.
Either during the implantation or after a short period of healing (2-4 weeks), the device will be turned on to start generating weak electrical impulses. The patient will feel them – VNS usually causes a low voice and a sore throat. After a day or two, the body will get used to the stimulator and these symptoms will subside. The device is then adjusted to gradually increase power. During this period, you should periodically visit your doctor to check the setting of the device. Once the ideal stimulation ‘recipe’ has been determined, combining the device’s power and on/off sequence, the neurologist’s observation returns to the normal frequency. The optimal performance of the implant is achieved in 4-8 months.
The VNS stimulator battery lasts for 10 years on average, although the exact life depends on how often it is used. After the VNS generator has been in operation for several years, more frequent monitoring, e.g. every 3 months, may be required to observe the battery life.
How do patients with a vagus stimulator live?
8 out of 10 patients with epilepsy report that VNS therapy has improved their quality of life.
By reducing the frequency and intensity of seizures, VNS therapy can make life more peaceful and predictable for patients with epilepsy. Positive effects include:
Improved attention span;
Improved memory;
Improvement in children’s verbal and reading skills;
Improved academic success;
Fewer mood swings;
Less anxiety;
Less depressive symptoms;
An easier period after a seizure.
At the same time, the presence of an implant inside the body brings certain adjustments to a person’s life. Depending on the model of the stimulator, an MRI may be contraindicated to the patient because of the danger of the metal components of the device interacting with the magnet. In the latest generation of vagus nerve stimulators, this disadvantage has been corrected and patients can undergo an MRI, but only on compatible, modern machines.
There are no contraindications to having an X-ray or CT scan with a vagus stimulator.
How effective is VNS treatment for epilepsy?
Already in the first 3 months of using vagus stimulation, the frequency of epileptic seizures is reduced by 28%;
After 6 months, seizure occurrence is reduced by 36%, after a year – by 52%, after 4 years – by 61%, after 8 years – by 76%;
Half of the patients report that their seizures have become milder and recovery takes less time;
About 6 in 10 report a reduction in anxiety about their seizures and an improvement in attention span;
1 in 10 manage to get rid of their attacks completely;
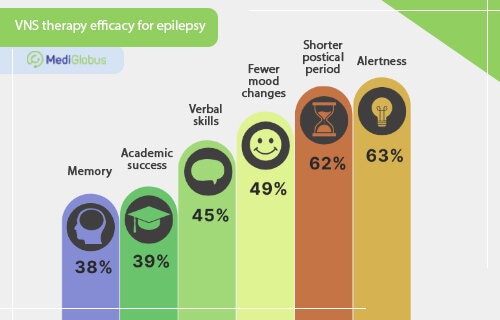
There is an improvement in alertness (58-63% of patients), a reduction in cluster seizure frequency (48-56%), a reduction in mood swings (43-49%), improvements in verbal communication (38-45%) and memory (29-38%), and progress in school or professional achievements (29-39%).
SIGN UP FOR EPILEPSY TREATMENT
Contact MediGlobus and we will recommend good neurology clinics and experienced doctors. To get a free consultation with our coordinating doctors, please click on the button below and fill in the form.
Indications, contraindications and side effects
VNS therapy is indicated for the treatment of all types of epilepsy that are resistant to standard drug therapy. These are considered to be cases where seizure control has not been achieved after using at least two tolerated drugs prescribed separately or together. The treatment can be used in both children and adults.
71% of patients who have vagus nerve stimulation are diagnosed with focal epilepsy.
Vagus nerve stimulation is also an alternative to surgical treatment for epilepsy in cases where surgery is contraindicated.
People with only one vagus nerve are not good candidates for VNS.
Also, people with a history of arrhythmia and bradycardia should weigh up the pros and cons well before surgery, and they should not use the autostimulation settings of the newer VNS models.
People with severe asthma or other breathing problems, sleep apnoea or some heart problems may be advised not to use vagus nerve stimulation. Sometimes similar medical problems may be worsened by the use of VNS.
The most common side effects of vagus nerve stimulation are:
Infection at the site of insertion of the stimulator;
Raspy voice;
Sore throat;
Coughing;
Shortness of breath.
Feedback on the vagus stimulator
Hospital: Liv Vadistanbul
Procedure: VNS installation
Patient’s age: 5 years
Patient from: Kropivnitsky
Lera: “My daughter was diagnosed with epilepsy when she was three. My husband and I were very frightened, and for a long time, we went to different doctors, tried different medications, keto diet… Nothing worked to stop the seizures. In the end, we thought long and hard about all the options and decided to take the risk with a VNS stimulator. I could hardly believe how amazing the results were. She is much calmer and more alert. Reading and communicating with other children has become much much easier for her… We have not regretted having this surgery for a single minute. Yes, VNS is not suitable for everyone, but for us, it was 100% the right decision.”
Clinics for treating epilepsy abroad
Summary
VNS therapy is a surgical treatment for resistant epilepsy. It involves attaching a stimulator that generates electrical impulses to the vagus nerve.
There are different models of vagus nerve stimulators. The latest generation machines have adaptive modes of operation and can recognise an impending seizure on their own to try to stop it.
VNS therapy reduces the frequency and intensity of epileptic seizures. As a consequence, the patient’s memory and concentration improve, their emotional state normalises, and the level of anxiety and depression decreases.
The effectiveness of VNS therapy in treating epilepsy is 52-76%.
Patients seek vagus nerve stimulation from specialist clinics in Turkey, Spain, Israel, and South Korea, such as Liv Vadistanbul, Teknon and SoonChunHyang.
SIGN UP FOR VNS THERAPY
To make an appointment for this procedure abroad, click on the button below and fill in the form. Our coordinators will call you back within 30 minutes. They will provide all necessary information and help with travel arrangements.
Sources:
- 1. Epilepsy Foundation
- 3. Epilepsy Society
- 4. Frontiers of Neurology: Responsive Vagus Nerve Stimulation for Drug Resistant Epilepsy: A Review of New Features and Practical Guidance for Advanced Practice Providers
- 5. Surgical Neurology International: Vagus nerve stimulation for epilepsy: A review of the peripheral mechanisms
- 6. Seizure: Learnings from 30 years of reported efficacy and safety of vagus nerve stimulation (VNS) for epilepsy treatment: A critical review
- 7. Frontiers of Neuroscience: Stimulation: Challenges for Translation to Clinical Practice











